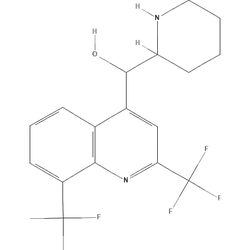
Mefloquine Stats & Data
Pharmacology
DrugBankDescription
Malaria is a protozoan disease that places an enormous burden on human health in endemic areas around the world. The 2020 World Health Organization malaria report indicates a 60% decrease in the global malaria fatality rate between 2000 to 2019. Despite this, malaria remains a significant cause of morbidity and mortality; 90% of deaths from malaria occur in Africa. Individuals at the highest risk for malaria are those in disease naïve populations, children under age 5, refugees in Central and Eastern Africa, nonimmune civilian and military travelers, pregnant women, and immigrants traveling to their place of origin. Mefloquine, commonly known as Lariam, is an antimalarial drug used for the prevention and treatment of malaria caused by infection with Plasmodium vivax and Plasmodium falciparum. The drug was initially discovered by the Walter Reed Army Institute of Research (WRAIR) during a malaria drug discovery program between 1963 until 1976. It was approved by the FDA in 1989, and was first marketed by Hoffman Laroche. This drug has been the subject of widespread controversy due to concerns regarding neurotoxic effects; product information warns of potential serious neuropsychiatric effects.
Mechanism of Action
The mechanism of action of mefloquine is not completely understood. Some studies suggest that mefloquine specifically targets the 80S ribosome of the Plasmodium falciparum, inhibiting protein synthesis and causing subsequent schizonticidal effects. There are other studies in the literature with limited in vitro data on mefloquine's mechanism of action.
Pharmacodynamics
Sporozoites located in the salivary glands of mosquitoes infected with malaria parasites are introduced into the bloodstream of a human host during mosquito feeding. These sporozoites rapidly invade the liver, where they mature into liver-stage schizonts, rupturing and releasing 2,000 - 40,000 merozoites that invade red blood cells. Mefloquine is an antimalarial drug acting as a blood schizonticide, preventing and treating malaria.
Metabolism
Mefloquine is heavily metabolized in the liver by the CYP3A4 enzyme. Two metabolites have been identified; the main metabolite, 2,8-bis-trifluoromethyl-4-quinoline carboxylic acid, which inactive against plasmodium falciparum. The second metabolite, an alcohol, is found in small quantities.
Absorption
Mefloquine is readily absorbed from the gastrointestinal tract; food significantly increases absorption and increases bioavailability by 40%. The bioavailability of tablets compared with the oral solution preparation of mefloquine is over 85%. Cmax is achieved in 6 to 24 hours in healthy volunteers after a single dose. Average blood concentrations range between 50 to 110 ng/ml/mg/kg. A weekly dose of 250 mg leads to steady-state plasma concentrations of 1000 to 2000 μg/L, after 7 to 10 weeks of administration.
Toxicity
The oral TDLO of mefloquine in humans is 11 mg/kg/2W (intermittent) and 880 mg/kg in the rat. Intraperitoneal LD50 in the rat is 130 mg/kg. Symptoms of an overdose with mefloquine may manifest as a worsening of adverse effects. In the case of an overdose, symptomatic and supportive care should be provided. There is no known antidote for an overdose with mefloquine. Monitor cardiac function by ECG, follow neuropsychiatric status for at least 24 hours, and provide treatment as required.
Indication
Mefloquine is indicated for the treatment of mild to moderate cases of malaria caused by Plasmodium falciparum and Plasmodium vivax. It is effective against chloroquine-resistant forms of Plasmodium falciparum. Mefloquine is also indicated for the prophylaxis of malaria caused by Plasmodium falciparum and Plasmodium vivax, including chloroquine-resistant forms of Plasmodium falciparum.
Half-life
The terminal elimination half-life of mefloquine ranges from 0.9 - 13.8 days, according to one pharmacokinetic review. In various studies of healthy adults, the mean elimination half-life of mefloquine varied between 2 and 4 weeks, with a mean half-life of approximately 21 days.
Protein Binding
The binding of mefloquine to plasma proteins is over 98%.
Elimination
Mefloquine is believed to be excreted in the bile and feces. In healthy volunteers who have achieved steady-state concentrations of mefloquine, the unchanged drug was excreted at 9% of the ingested dose, and excretion of its carboxylic metabolite under was measured at 4% of the ingested dose. Concentrations of other metabolites could not be determined.
Volume of Distribution
The apparent volume of distribution is in healthy adults is about 20 L/kg with wide tissue distribution. Various estimates of the total apparent volume of distribution range from 13.3 to 40.9L/kg. Mefloquine can accumulate in erythrocytes that have been infected with malaria parasites.
Clearance
The systemic clearance of mefloquine ranges from 0.022 to 0.073 L/h/kg, with an increased clearance during pregnancy. Prescribing information mentions a clearance rate of 30 mL/min.
Receptor Profile
Receptor Actions
Receptor Binding
Tolerance & Pharmacokinetics
drugs.wikiExperience Report Analysis
ErowidDemographics
Gender Distribution
Age Distribution
Reports Over Time
Effect Analysis
ErowidEffects aggregated from 3 experience reports (3 Erowid)
Effect Sentiment Distribution
Confidence Distribution
Positive Effects 0
Adverse Effects 1
Harm Reduction
drugs.wikiBoxed/major warnings emphasize that psychiatric symptoms (e.g., acute anxiety, depression, restlessness) or neurologic/vestibular symptoms (e.g., dizziness, loss of balance, tinnitus) can begin early and may persist; discontinue mefloquine at the first occurrence of such prodromal symptoms and do not re-challenge. Concomitant or closely timed use (up to ~15 weeks after last dose, reflecting the long half-life) with halofantrine or ketoconazole is specifically warned against due to life‑threatening QTc prolongation; other QT‑affecting drugs warrant caution. A history of major psychiatric disorders (depression, GAD, psychosis, schizophrenia) or seizures is a contraindication to prophylactic use; hypersensitivity to quinine/quinidine is also a contraindication. Due to vestibular and neuropsychiatric risks, use caution with activities requiring alertness and fine motor control (driving, piloting, operating machinery, diving). Start prophylaxis at least 1 week before travel (2 weeks often recommended when feasible) to assess tolerability; continue for 4 weeks after return. Food increases absorption (~40%); take weekly doses with food and water, and avoid alcohol around dosing to reduce CNS side effects. Mefloquine is primarily metabolized by CYP3A4 and is a P‑gp substrate/inhibitor; strong CYP3A4 inhibitors raise exposure and inducers (e.g., rifampin) lower exposure and may compromise efficacy. With chronic/long‑term use, liver enzyme elevations occur in a subset of users; periodic LFT monitoring is advised in prolonged courses and elimination is prolonged in hepatic impairment. Women and individuals with low BMI may be at higher risk for certain neuropsychiatric adverse effects in some cohorts; concurrent alcohol or other chronic medications has been associated with increased adverse event reporting. Breastmilk contains low mefloquine concentrations insufficient to protect an infant; breastfeeding infants require their own antimalarial prophylaxis where indicated.
References
Data Sources
Cited References
- DrugBank: Mefloquine Hydrochloride
- FDA Mefloquine Label (2008)
- Karle et al. 2014: Mefloquine and Psychotomimetics Share Neurotransmitter Receptor Interactions
- Mayo Clinic: Mefloquine Dosage
- MedlinePlus: Mefloquine Drug Information
- NCBI Bookshelf: Assessment of Long-Term Health Effects of Antimalarial Drugs
- PubChem: Mefloquine
- DrugBank: Mefloquine syndrome
- DrugBank: Mefloquine side effects
Drugs.wiki References
- NCBI Bookshelf: Assessment of Long-Term Health Effects of Antimalarial Drugs – Mefloquine chapter (2020)
- DrugBank: Mefloquine monograph (DB00358)
- DrugBank article: Cardiotoxicity of antimalarial drugs (Lancet Infect Dis 2007)
- NCBI Bookshelf: LiverTox – Mefloquine (revised)
- NCBI Bookshelf: LactMed – Mefloquine (2025 update)