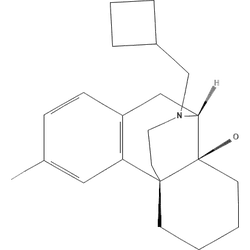
Butorphanol Stats & Data
Oc1ccc2CC3N(CC4CCC4)CCC4(CCCCC34O)c2c1IFKLAQQSCNILHL-QHAWAJNXSA-NPharmacology
DrugBankDescription
A synthetic morphinan analgesic with narcotic antagonist action. It is used in the management of severe pain.
Mechanism of Action
The exact mechanism of action is unknown, but is believed to interact with an opiate receptor site in the CNS (probably in or associated with the limbic system). The opiate antagonistic effect may result from competitive inhibition at the opiate receptor, but may also be a result of other mechanisms. Butorphanol is a mixed agonist-antagonist that exerts antagonistic or partially antagonistic effects at mu opiate receptor sites, but is thought to exert its agonistic effects principally at the kappa and sigma opiate receptors.
Pharmacodynamics
Butorphanol is a synthetic opioid agonist-antagonist analgesic with a pharmacological and therapeutic profile that has been well established since its launch as a parenteral formulation in 1978. The introduction of a transnasal formulation of butorphanol represents a new and noninvasive presentation of an analgesic for moderate to severe pain. This route of administration bypasses the gastrointestinal tract, and this is an advantage for a drug such as butorphanol that undergoes significant first-pass metabolism after oral administration. The onset of action and systemic bioavailability of butorphanol following transnasal delivery are similar to those after parenteral administration. Butorphanol blocks pain impulses at specific sites in the brain and spinal cord.
Metabolism
Extensively metabolized in the liver. The pharmacological activity of butorphanol metabolites has not been studied in humans; in animal studies, butorphanol metabolites have demonstrated some analgesic activity.
Absorption
Rapidly absorbed after intramuscular injection and peak plasma levels are reached in 20-40 minutes. The absolute bioavailability is 60-70% and is unchanged in patients with allergic rhinitis. In patients using a nasal vasoconstrictor (oxymetazoline) the fraction of the dose absorbed was unchanged, but the rate of absorption was slowed. Oral bioavailability is only 5-17% because of extensive first-pass metabolism.
Toxicity
The clinical manifestations of butorphanol overdose are those of opioid drugs in general. The most serious symptoms are hypoventilation, cardiovascular insufficiency, coma, and death.
Indication
For the relief of moderate to severe pain.
Half-life
The elimination half-life of butorphanol is about 18 hours. In renally impaired patients with creatinine clearances <30 mL/min the elimination half-life is approximately doubled. After intravenous administration to patients with hepatic impairment, the elimination half-life of butorphanol was approximately tripled.
Elimination
Butorphanol is extensively metabolized in the liver. Elimination occurs by urine and fecal excretion.
Clearance
* 99 +/- 23 L/h Young with IV 2 mg * 82 +/- 21 Eldery with IV 2 mg
Effect Profile
Curated + 12 ReportsStrong euphoria with moderate itching/nausea, mild pain relief, low sedation
Tolerance & Pharmacokinetics
drugs.wikiTolerance Decay
Patterns are extrapolated from general opioid tolerance behavior and limited user reports. κ‑agonist dysphoria can reduce compulsive redosing for some, but physiological tolerance and dependence can still develop after several consecutive days. Data quality is low; individual variation is high.
Cross-Tolerances
Experience Report Analysis
ErowidDemographics
Gender Distribution
Age Distribution
Reports Over Time
Effect Analysis
ErowidEffects aggregated from 12 experience reports (12 Erowid)
Effect Sentiment Distribution
Confidence Distribution
Positive Effects 5
Adverse Effects 2
Real-World Dose Distribution
62K DosesFrom 13 individual dose entries
Oral (n=5)
Form / Preparation
Most common forms and preparations reported
Redose Patterns
Redosing behavior across 10 reports
Opioid Equivalence (MME)
NIH HEAL 2024 & CDC 2022Butorphanol 1.42 mg oral ≈ 10 mg Morphine oral
Harm Reduction
drugs.wiki- Butorphanol is a mixed agonist–antagonist opioid: κ-opioid receptor agonism with partial μ-agonist/antagonist effects. This profile can antagonize effects of full μ-agonists (morphine, oxycodone, methadone), which may precipitate acute withdrawal in physically dependent people; avoid using butorphanol to 'boost' or on top of maintenance/full agonists. Carry naloxone if opioids are used in any context.
- Intranasal bioavailability is high relative to oral (approx. 70% vs ~17%), so intranasal dosing is more potent than the same oral milligram amount. Start with the lowest effective dose and wait at least a full peak window (≥90 minutes) before redosing to avoid stacking.
- Combining with other CNS depressants (alcohol, benzodiazepines, barbiturates, gabapentinoids, Z‑drugs) markedly increases risk of respiratory depression, accidental injury, and fatal overdose. If any sedatives are on board, reduce dose substantially, avoid redosing, and do not use alone.
- κ‑agonism commonly produces dysphoria, anxiety, and ‘spacey’ or unpleasant headspace in some users; this can limit compulsive redosing but also increases risk of panic, confusion, and dangerous behavior in unfamiliar settings. Avoid operating vehicles or hazardous equipment during and after effects until fully alert.
- Effect duration is short relative to elimination; sedation and impaired coordination can outlast perceived analgesia. Plan for residual impairment (2–6 h) and avoid rapid redose cycles.
- Oral use is inefficient and unpredictable because of extensive first‑pass metabolism. If oral dosing is attempted, expect weaker, delayed effects and higher interindividual variability.
- Injection carries infection risks (skin/soft‑tissue infection, bacteremia, endocarditis). Use new sterile equipment each time, rotate sites, and avoid non‑sterile/veterinary preparations for human injection.
- Hepatic or renal impairment significantly prolongs elimination and increases exposure; use smaller doses with longer intervals or avoid non‑medical use altogether in these conditions. Older adults also clear butorphanol more slowly; start low and go slow.
- Because butorphanol can block or blunt full μ‑agonists, it may reduce the effectiveness of opioids given for emergency pain control for several hours; disclose recent use to clinicians.
- Intranasal solutions are often 10 mg/mL; product-specific sprays can deliver different mg per actuation. Verify the exact per‑spray amount before use to prevent unintended high doses.
References
Drugs.wiki References
- DrugBank: Butorphanol (DB00611) – identification, mechanism, bioavailability, interactions, and half-life notes
- LactMed (NCBI Bookshelf): Butorphanol – oral (~17%) vs intranasal (~70%) bioavailability; breastfeeding safety summary (Updated Feb 15, 2025)
- LiverTox (NCBI Bookshelf): Butorphanol – mixed agonist–antagonist profile; availability; adverse effects overview; hepatic safety
- NCBI Bookshelf – Self-Administered Drug Treatments for Acute Migraine: Butorphanol adverse event profile (dizziness, drowsiness, nausea, sweating, confusion, euphoria)
- StatPearls (NCBI Bookshelf): Opioid Toxicity – additive risk with benzodiazepines and other depressants; naloxone considerations
- WHO/NCBI Bookshelf: Pharmacological management of cancer pain – note that opioid antagonists/partial agonists can precipitate opioid withdrawal
- Bluelight: Dangerous Drug Combos – anecdotal warning that agonist/antagonists (e.g., Stadol) can precipitate withdrawal in methadone‑tolerant individuals