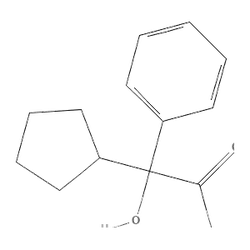
Effect Profile
CuratedLow visuals, body load, and headspace
Tolerance & Pharmacokinetics
drugs.wikiTolerance Decay
No systematic data on tolerance. Given the prolonged single‑exposure intoxication and absence of repeated recreational use, practical tolerance build is unlikely to be characterized. Conservatively assume at least several weeks before baseline cognition and cholinergic tone normalize after severe intoxication.
Harm Reduction
drugs.wikiRationale: Edgewood/NRC analyses identify EA-3167 as one of the longest-lasting anticholinergic incapacitating glycolates, with incapacitation lasting roughly 4–10 days and peak delirium within the first 1–3 days; this extreme duration creates unusually high risks of dehydration, hyperthermia, wandering/accidents, and inability to self‑care. Rationale: Two accidental high-dose exposures to EA‑3167 described in NRC review showed mild but noticeable cognitive impairment persisting for approximately six months before full recovery, underscoring the potential for protracted neurocognitive after‑effects following severe intoxication. Rationale: Standard toxicology guidance for anticholinergic syndrome supports aggressive supportive care (cooling, IV fluids, urinary retention management) and careful use of IV benzodiazepines for agitation; physostigmine is indicated for severe, confirmed anticholinergic delirium but requires cardiac monitoring and repeat dosing due to short action. Avoid physostigmine in mixed/unknown overdoses (e.g., TCA co‑ingestion). Rationale: Additive anticholinergic burden with first‑generation antihistamines, tricyclics, and phenothiazines can worsen delirium, tachycardia, and arrhythmia risk; several carry QT‑prolongation liabilities. Rationale: Combining with alcohol, opioids, or unsupervised benzodiazepines increases sedation/blackout and aspiration/trauma risk during delirium; clinical benzodiazepine use differs because it is titrated IV with monitoring in emergency settings. Rationale: Onset to incapacitation around 1–2 h and long distribution into CNS imply that delayed care seeking is common; having sober supervision and rapid access to emergency services is essential if exposure is suspected. Rationale: Because effects outlast likely plasma kinetics, serum levels are a poor guide to clinical severity; treatment is guided by toxidrome. Rationale: Due to extreme hazard profile, non‑medical use is effectively non‑existent; information is presented solely to prevent harm in accidental or historical exposure contexts.
References
Drugs.wiki References
- NRC/NCBI Bookshelf – DIGEST REPORT—Anticholinergic Chemicals (includes EA‑3167 data)
- NRC/NCBI Bookshelf – Possible Long-Term Health Effects… (full PDF)
- NCBI Bookshelf – MASTER FILE—Anticholinergic Chemicals
- StatPearls/NCBI – Anticholinergic Toxicity (management incl. benzodiazepines and physostigmine)
- StatPearls/NCBI – Antihistamines (anticholinergic burden, QT considerations)
- StatPearls/NCBI – Antipsychotic Medications (contraindications with anticholinergics)
- Erowid – BZ Basics (context on glycolate incapacitating agents and lack of recreational market)
- Bluelight – Dangerous Drug Combos (depressant synergies)